Medical Device Corrosion Testing per ASTM F2129
The human body and its immune and inflammatory mechanisms can create an aggressive environment for metallic implants resulting in implant rejection and failure (Gilbert, Corrosion, 2017;73(12):1478-1495). In vitro testing of small implants is typically performed per ASTM F2129 to mitigate these risks. While this testing helps determine implant susceptibility to corrosion, it does not take into account the effects of cells, proteins, and other biological effects that implants will experience in vivo.
Despite its limitations, ASTM F2129 has undergone several revisions since its original publication in 2001 to better assist medical device manufacturers in assessing their small implants’ resistance to pitting and crevice corrosion. The standard provides a test method for conducting cyclic (forward and reverse) potentiodynamic polarization measurements on whole devices in their final form and finish.
In the sections below, we describe the test methods, apparatus, results and acceptance criteria used in vitro corrosion testing of small implants.
Test Apparatus
A typical multiport electrochemical test cell is used for testing. It has inflow/outflow ports for the nitrogen gas and heated water circulation, ports for the reference, graphite counter and working/sample electrodes, and an inner chamber for the saline bath.
Additional components include potentiostat, computer, pH meter, nitrogen tank, water pump, conductive epoxy with UV lamp and mask for curing, and stainless steel wire for sample attachment. Reagents such as phosphate buffered saline are used for the bath, and isopropyl alcohol and type II reagent grade water for sample rinsing. Optical and electron scanning microscopes are used for pre-and post-test inspections.
Test Method
Table 1 provides a brief terminology summary; for further details consult the ASTM F2129 standard.

Briefly, the implant is held in saline at 37±1°C with a starting pH at 7.4±0.2 in the setup shown on the right. A potential is introduced between the implant and a reference electrode and ramped up to the above physiological potentials. A breakdown will typically will result in a rapid increase in current density, as evidenced by the output plot of potential vs. log current density. The total surface area of the sample exposed to the solution needs to be calculated or estimated so that the current density generated by the sample can be determined.
Samples are prepared for testing and thoroughly inspected. Any preconditioning should be performed as it can impact the behavior of the implants. Conductive epoxy is used as the interface to the sample (specimen holders vary depending on the device type), connected to a potentiostat through a wire, and resistance is checked to ensure a good connection. The test cell is filled with saline (minimum of 500 mL, typically 1L), heated to the target temperature, and nitrogen gas flow at 150 mL/min is initiated. Nitrogen gas flow is used to deaerate the solution and lower dissolved oxygen concentration to decrease the potential at which oxidation and reduction currents are equal.
Temperature, pH, and nitrogen gas flow time (30 min minimum) are recorded, then the device is rinsed and inserted in the test cell with the wire. Saline is added into the reference electrode holder, and the electrode is inserted at 5mm or less from the sample, but not in contact with the sample. The nitrogen purge is continued throughout the test. The open circuit test is initiated, and Er is recorded after 1 hour. Then, the cyclic polarization test is initiated at a 1 mV/s scan rate by setting Ei and Ef to Er. The cyclic polarization is closely monitored; if a current density increase larger than two decades occurs, voltage is reversed.
When the test is completed, the final temperature, pH, Er, Eb, Ef, and Ep are recorded. The sample is removed from the test and rinsed, the wire is clipped ~1 inch above the sample, and the sample is stored for further post-test inspection. While the standard does not indicate how many samples should be tested, we typically see 3-8 samples per surface finish.
Test Results
Test conditions are recorded for each sample: nitrogen flow time, initial temperature, initial pH, final temperature, and final pH. Sample test results are typically provided in tabular and graphical formats. Pre- and post-test observations and inspection results are also provided.
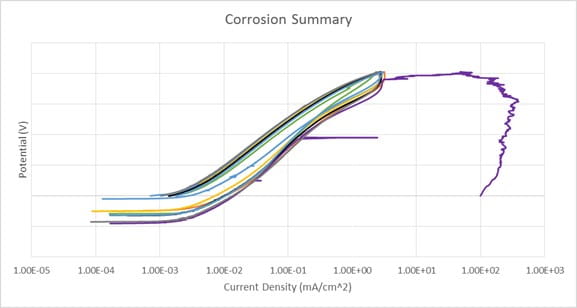
The graph above shows results from a corrosion test of 8 samples of a nitinol device plotted as potential (mV) vs. log current (A). Results show consistency between the 8 samples; the purple data set with the increase in current density is an example of a breakdown potential.
Acceptance Criteria
ASTM F2129 does not define acceptance criteria but identifies Eb as the critical data point above which pits nucleate and grow. Therefore, the higher the Eb is, the more resistant the metal is to pitting corrosion. It is also recommended that Eb values are compared to those of predicate devices that have demonstrated good corrosion resistance in vivo as a reference. Device manufacturers define the acceptance criteria for their implants. In our experience, acceptable Eb values are most commonly set above 300 mV, and they are often set at much higher threshold values.
Consultation
We often perform corrosion testing on medical devices to characterize their corrosion potential. If you would like more information about our medical device corrosion testing services, or for assistance with your device’s corrosion and/or fatigue testing, contact our Engaged Experts to discuss how we can help.
Element offers the broadest scope of medical device testing, so if you are looking for services such as package testing, microbiological analysis, accelerated aging-shelf life testing, or EMC/EMI testing, contact us to connect with the right lab.
Find related Resources
Related Services

Medical Device Testing
As a comprehensive testing partner, you’ll enjoy the benefit of a single supplier source for all of your testing needs, from mechanical testing and environmental simulation to EMC and wireless device testing.

Reusable Medical Device Life Cycle Validation
Our medical device experts evaluate the environmental impact on the identification markings and function of reusable medical instruments after repeated autoclave sterilization cycles.

Medical Device Testing Tips
Preparing for a medical device testing program can be a challenge for many manufacturers, especially if it is a new or novel product or if time is limited. Our medical device experts share their testing tips and best practices.
Sign Up for Free Resources
Visit Element's email subscription center to receive the latest industry news, technical whitepapers, case studies, webinars, and upcoming events.
